Work on similar viruses is giving researchers clues to develop drugs against the disease
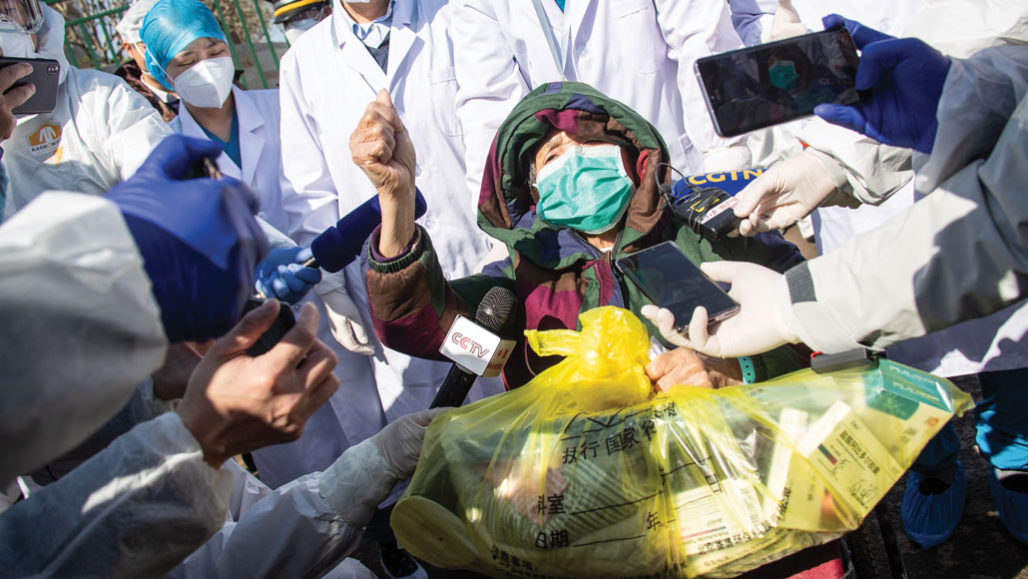
As the new coronavirus makes its way around the world, doctors and researchers are searching for repurposed drugs to treat the ill and stop the spread of the disease, which has already killed more than 3,000 people since its introduction in Wuhan, China, in December.
The culprit virus is in the same family as the coronaviruses that caused two other outbreaks, severe acute respiratory syndrome and Middle East respiratory syndrome. But the new coronavirus may be more infectious. In early March, the number of confirmed cases of the new disease, called COVID-19, had exceeded 100,000, far surpassing the more than 10,600 combined total cases of SARS and MERS.
Health officials are mainly relying on quarantines to try to contain the virus’ spread. Such low-tech public health measures were effective at stopping SARS in 2004, Anthony Fauci, director of the U.S. National Institute of Allergy and Infectious Diseases, said January 29 in Arlington, Va., at the annual American Society for Microbiology’s Biothreats meeting.
But stopping the new virus may require a more aggressive approach. In China alone, about 300 clinical trials are in the works to treat sick patients with standard antiviral therapies, such as interferons, as well as stem cells and traditional Chinese medicines including acupuncture, and blood plasma from people who have already recovered from the virus.
Researchers are not stopping there. They also are working to develop drugs to treat infections and vaccines to prevent them (SN: 3/14/20, p. 6). But creating therapies against new diseases often takes years, if not decades. With this new coronavirus, now known as SARS-CoV-2, nobody wants to wait that long. Thanks to their experience developing treatments against the MERS coronavirus, as well as other diseases, such as HIV, hepatitis C, influenza, Ebola and malaria, researchers are moving quickly to see what they can borrow to help patients sooner.
Finding new uses for old drugs is a good strategy, especially when racing to fight a fast-moving disease for which there is no treatment, says Karla Satchell, a microbiologist and immunologist at Northwestern University Feinberg School of Medicine in Chicago.
“Repurposing drugs is absolutely the best thing that could happen right now,” Satchell says. Potentially, drugs that combat HIV or hepatitis C might be able to put the new coronavirus in check too. “Those drugs exist. They’ve been produced. They’ve been tested in patients,” she says. Although these drugs aren’t approved to treat the new coronavirus disease, they’re a great place to start. One of the most promising candidates, however, hasn’t yet been approved for any disease.
Early focus
Scientists have been quick to reveal the new coronavirus’ secrets. When SARS emerged in 2002, researchers took about five months to get a complete picture of the virus’s genetic makeup, or genome. With the new virus, Chinese health officials first reported a cluster of mysterious pneumonia cases in Wuhan to the World Health Organization on December 31. By January 10, the new coronavirus’s full genome was made available to researchers worldwide in public databases.
A virus’s genome is one of the most valuable tools scientists have for understanding where the pathogen came from, how it works and how to fight it. The first thing that coronaviruses have in common is that their genetic material is RNA, a chemical cousin to DNA.
Researchers immediately began comparing the new coronavirus’s genome with SARS and MERS viruses and other RNA viruses to determine whether drugs developed to combat those disease-causing organisms would work against the new threat. As a result, some potential Achilles’ heels of SARS-CoV-2 have already come to light.
One target is the virus’s main protein-cutting enzyme, called M protease. RNA viruses often make one long string of proteins that later get cut into individual proteins to form various parts of the virus. In the new coronavirus, the M protease is one of 16 proteins that are linked like beads on a string, says Stephen Burley, an oncologist and structural biologist at Rutgers University in Piscataway, N.J.
The virus can mature and infect new cells only if M protease can snip the string of proteins free, he says. Stop the protease from cutting and the virus can’t reproduce, or replicate.
Existing drugs might be able to stop the virus’s M protease, two research groups proposed online January 29 at bioRxiv.org. One group suggested four drugs, including one used to treat hepatitis C and two aimed at HIV. A second group named 10 candidates: including an antinausea medication, an antifungal drug and some cancer-fighting drugs.
HIV and hepatitis C are both RNA viruses that need a protease to cut proteins free from long chains. Drugs that inhibit those proteases can reduce levels of the HIV and hepatitis C viruses to undetectable. Some of those drugs are now being tested against the new coronavirus in clinical trials in China.
The HIV drug Kaletra, also called Aluvia, is a combination of two protease inhibitors, lopinavir and ritonavir. Kaletra’s maker, the global pharmaceutical company AbbVie, announced on January 26 that it is donating the drug to be tested in COVID-19 patients in China. Kaletra will be tested alone or in combination with other drugs. For instance, researchers may combine Kaletra with Arbidol, a drug that prevents some viruses from fusing with and infecting human cells. Arbidol may be tested on its own as well.
But the HIV drugs may not work against the new virus because of two differences in the proteases. The coronavirus protease cuts proteins in different spots than the HIV protease does, say Guangdi Li of the Xiangya School of Public Health of Central South University in Changsha, China, and Erik De Clercq, a pioneer in HIV therapy at KU Leuven in Belgium. Secondly, the HIV drugs were designed to fit a pocket in HIV’s protease that doesn’t exist in the new coronavirus’s protease, the researchers reported February 10 in Nature Reviews Drug Discovery.
Yet a few anecdotal accounts suggest the HIV drugs may help people with COVID-19 recover. Doctors at Rajavithi Hospital in Bangkok reported in a press briefing February 2 that they had treated a severely ill 70-year-old woman with high doses of a combination of lopinavir and ritonavir and the anti-influenza drug oseltamivir, which is sold as Tamiflu. Within 48 hours of treatment, the woman tested negative for the virus.
Her recovery may be due more to the HIV drugs than to oseltamivir. In 124 patients treated with oseltamivir at Zhongnan Hospital of Wuhan University, “no effective outcomes were observed,” doctors reported on February 7 in JAMA. Clinical trials in which these drugs are given to more people in carefully controlled conditions are needed to determine what to make of those isolated reports.
Viral weak spots
Researchers may be able to exploit a second weakness in the virus: its copying process, specifically the enzymes known as RNA-dependent RNA polymerases that the virus uses to make copies of its RNA. “Those enzymes are absolutely essential,” says Mark Denison, an evolutionary biologist at Vanderbilt University School of Medicine in Nashville. If the enzyme doesn’t work, “you can’t make new virus.”
Denison and colleagues have been testing molecules that muck with the copying machinery of RNA viruses. The molecules mimic the nucleotides that RNA polymerases string together to make viral genomes. Researchers have tested chemically altered versions of two RNA nucleotides — adenosine and cytidine — against a wide variety of RNA viruses in test tubes and in animals. The molecules “get incorporated into the viral RNA and either stop it from growing or they damage it by introducing mutations,” Denison says.
One of the molecules that researchers are most excited about is an experimental drug called remdesivir. The drug is being tested in people with COVID-19 because it can stop the MERS virus in the lab and in animal studies. The drug has also been used in patients with Ebola, another RNA virus.
Remdesivir has been given to hundreds of people infected with Ebola, without causing serious side effects, but the drug hasn’t been as effective as scientists had hoped, virologist Timothy Sheahan of the University of North Carolina at Chapel Hill said January 29 at the Biothreats meeting. In a clinical trial in Congo, for example, about 53 percent of Ebola patients treated with remdesivir died, researchers reported November 27 in the New England Journal of Medicine. That’s better than the 66 percent of infected people killed in the ongoing Ebola outbreak, but other drugs in the trial were more effective.
Several tests of remdesivir in lab animals infected with MERS have researchers still hopeful when it comes to the new coronavirus. In studies in both rhesus macaques and mice, remdesivir protected animals from lung damage whether the drug was given before or after infection. Molecular pathologist Emmie de Wit of NIAID’s Laboratory of Virology in Hamilton, Mont., and colleagues reported the monkey results February 13 in the Proceedings of the National Academy of Sciences.
“Remdesivir appears to be one of the most promising antiviral treatments tested in a nonhuman primate model to date,” the team wrote. The results also suggest remdesivir given before infection might help protect health care workers and family members of infected people from getting severe forms of the disease, Sheahan says.
Denison, Sheahan and colleagues tested remdesivir on infected human lung cells in the lab and in mice infected with MERS. Remdesivir was more potent at stopping the MERS virus than HIV drugs and interferon-beta, the researchers reported January 10 in Nature Communications.
But the question is still open about whether remdesivir can stop the new coronavirus.
In lab tests, it can. Both remdesivir and the antimalaria drug chloroquine inhibited the new virus’s ability to infect and grow in monkey cells, virologist Manli Wang of the Wuhan Institute of Virology of the Chinese Academy of Sciences and colleagues reported February 4 in Cell Research. Remdesivir also stopped the virus from growing in human cells. Chloroquine can block infections by interfering with the ability of some viruses — including coronaviruses — to enter cells. Wang and colleagues found that the drug could also limit growth of the new coronavirus if given after entry. Chloroquine also may help the immune system fight the virus without the kind of overreaction that can lead to organ failure, the researchers propose.
In China, remdesivir is already being tested in patients. And NIAID announced February 25 that it had launched a clinical trial of remdesivir at the University of Nebraska Medical Center in Omaha. The first enrolled patient was an American evacuated from the Diamond Princess cruise ship in Japan that had been quarantined in February because of a COVID-19 outbreak.
Ultimately, nearly 400 sick people at 50 centers around the world will participate in the NIAID trial, which will compare remdesivir with a placebo. The trial may be stopped or altered to add other drugs depending on results from the first 100 or so patients, says Andre Kalil, an infectious disease physician at the University of Nebraska Medical Center.
Researchers considered many potential therapies, but based on results from the animal and lab studies, “remdesivir seemed to be the one that was more promising,” Kalil says.
In the early patient studies, figuring out when to give remdesivir to patients might not be easy, Sheahan says. Often drugs are tested on the sickest patients. For example, those in the NIAID trial must have pneumonia to participate. By the time someone lands in the intensive care unit with COVID-19, it may be too late for remdesivir to combat the virus, Sheahan says. It may turn out that the drug works best earlier in the disease, before viral replication peaks.
“We don’t know because it hasn’t really been evaluated in people how remdesivir will work, or if it will work at all,” Sheahan cautions.
The drug seems to have helped a 35-year-old man in Snohomish County, Wash., researchers reported January 31 in the New England Journal of Medicine. The man had the first confirmed case of COVID-19 in the United States. He developed pneumonia, and doctors treated him with intravenous remdesivir. By the next day, he was feeling better and was taken off supplemental oxygen.
That’s just one case, and the company that makes remdesivir has urged caution. “Remdesivir is not yet licensed or approved anywhere globally and has not been demonstrated to be safe or effective for any use,” the drug’s maker, biopharmaceutical company Gilead Sciences, headquartered in Foster City, Calif., said in a statement on January 31.
But global health officials are eager to see the drug tested in people. “There’s only one drug right now that we think may have real efficacy, and that’s remdesivir,” WHO’s assistant director-general Bruce Aylward said during a news briefing on February 24. But researchers in China are having trouble recruiting patients into remdesivir studies, partly because the number of cases has been waning and partly because too many trials of less-promising candidates are being offered. “We have got to start prioritizing enrollment into those things that may save lives and save them faster,” Aylward said.
Decoy defense
Another strategy for combating COVID-19 involves distracting the virus with decoys. Like the SARS virus, the new virus enters human cells by latching on to a protein called ACE2. The protein studs the surface of cells in the lungs and many other organs. A protein on the surface of the new virus binds to ACE2 10 to 20 times as tightly as the SARS protein does.
Researchers at Vienna-based Apeiron Biologics announced February 26 that they would use human ACE2 protein in a clinical trial against the new coronavirus. When released into the body, the extra ACE2 acts as a decoy, glomming on to the virus, preventing it from getting into cells.
ACE2 isn’t just a virus’s doorway to infection. Normally, it helps protect the lungs against damage, says Josef Penninger, an immunologist at the University of British Columbia in Vancouver and a cofounder of Apeiron. Penninger and colleagues reported the protein’s protective qualities, based on studies with mice, in Nature in 2005.
During a viral infection, the protein is drawn away from the cell surface and can’t offer protection. Penninger thinks that adding in extra ACE2 may help shield the lungs from damage caused by the virus and by immune system overreactions. The protein is also made in many other organs. Penninger and colleagues are testing whether the new virus can enter other tissues, which might be how the virus leads to multiple organ failures in severely ill people.
The decoy protein drug, called APN01, has already been through Phase I and Phase II clinical testing. “We know it’s safe,” Penninger says. Now researchers just need to determine whether it works.
Persistent problem solving
No one knows whether any of these approaches can help stem the spread of COVID-19.
“Right now, we need lots of people working with lots of ideas,” Satchell says. Similarities between the viruses that cause SARS and COVID-19 may mean that some drugs could work against both. “There is a hope that several small molecules that were identified as inhibitors of the SARS protease would represent reasonable starting points for trying to make a drug for the 2019 coronavirus,” Burley says.
“The open question is, can you produce a drug that is both safe and effective quickly enough to have an impact?” SARS was stopped by traditional infection-control measures in 2004, before any virus-fighting drugs made it through the development pipeline.
But had a decision been made then to spend $1 billion to make a safe and effective drug against SARS, Burley says, such a drug might be working now against the new coronavirus, eliminating the need to spend hundreds of billions of dollars to contain this new infection.
An investment in SARS would not have paid off for people with MERS, which is still a danger in the Middle East. The MERS virus is too different from SARS at the RNA level for SARS drugs to work against it.
But a future coronavirus might emerge that is similar enough to SARS and SARS-CoV-2 to be worth the risk, Burley says. Even if the current outbreak dwindles and disappears, he says, governments and companies should keep investing in drugs that can stop coronaviruses.
“I’m quite certain that the economic impact of the epidemic is going to run into the hundreds of billions,” he says. “So you would only need a 1 percent chance of something that was treatable with the drug to show up in the future to have made a good investment.”











![Hotstar Premium Cookies 2019 [*100% Working & Daily Updated*] Hotstar Premium Cookies 2019 [*100% Working & Daily Updated*]](https://tahav.com/wp-content/uploads/2019/11/Hotstar-Premium-Cookies-Free-100x70.jpg)



